
STAGE WEBINAR OUTLINES POLICY CONSIDERATIONS TO IMPROVE HEALTH OUTCOMES
The first STAGE Science to Policy webinar brought together researchers, policymakers, clinicians, and individuals with lived experience to examine healthy ageing through a systems lens. Across all presentations, a consistent message emerged. Healthy ageing is not only a biomedical issue. It is shaped by interconnected biological, social, environmental, and policy factors across the life course. To improve outcomes, research and policy must move beyond fragmented approaches and integrate lived experience as a core component of design and implementation.
Professor Sylvain Sebert, STAGE Project Coordinator, provided the overarching framework for the discussion. He positioned healthy ageing as a dynamic system influenced by factors operating at multiple levels, from individual biology to societal structures. As highlighted in the opening session, healthy ageing is a lifelong process shaped by time, place, and social context, rather than a condition that begins in older age. This perspective challenges traditional models that focus on single diseases or late-life interventions. Instead, it supports a life-course approach that emphasises prevention, early action, and coordination across sectors.
Data presented in the webinar reinforced the urgency of this shift. A large proportion of adults over 50 already live with chronic conditions, and many experience multimorbidity, defined as two or more chronic diseases occurring simultaneously. At the same time, Europe’s ageing population is growing rapidly, with a projected 56.1 percent increase in those aged 75 to 84 by 2050. These trends highlight that current health systems, which are often organised around single conditions and episodic care, are ill-equipped to respond.
SURVEY OF PEOPLE AGED OVER 50
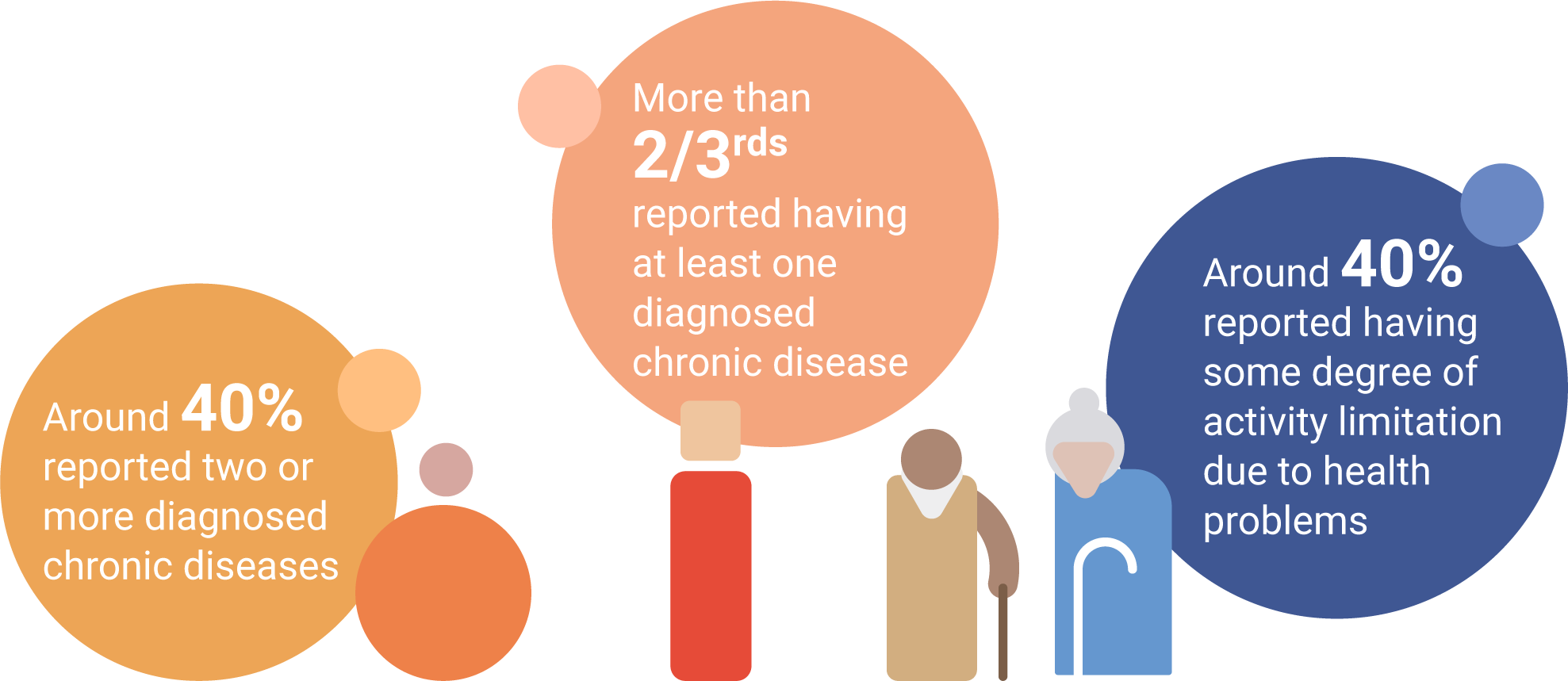
Reference: Survey of Health, Ageing and Retirement in Europe (SHARE) which collects data from over 50s in 11 European countries
Critical insights came from a lived-experience perspective. Mari-Mette Graff’s presentation made clear that people living with obesity and multi-morbidity often navigate highly fragmented systems. Individuals frequently act as their own care coordinators, managing multiple appointments, providers, and treatment plans. This fragmentation creates a significant burden and can undermine effective care.
Mari-Mette also highlighted less obvious barriers. These include stigma related to weight and age, digital exclusion, and feelings of guilt that discourage people from seeking care. Importantly, these factors are rarely included in traditional research or policy frameworks. Yet, they directly affect health behaviours, access to services, and long-term health and social outcomes.
Healthy ageing was defined as maintaining functional ability that enables well-being, rather than simply preventing disease. Dr. Yongjie Yon shared that the “Ageing is Living” strategy proposed by WHO Europe focuses on prevention, integrated care systems, age-friendly environments, and addressing ageism. It also emphasises the importance of data systems, stakeholder engagement, and cross-sector collaboration.

Panellists also emphasised that current health systems often focus on short-term, individual interventions, while more comprehensive chronic disease strategies require ongoing investment and system redesign. At the same time, practical examples shared by Dr. Jean O’Connell during the discussion showed that integrated care is possible. National and community initiatives, such as social prescribing, chronic disease management programmes, community specialist teams, and collaborations between healthcare and social services, demonstrate how coordinated models can enhance prevention, early detection, and long-term care.

First, health systems need to move towards integrated, multidisciplinary models of care that address multiple conditions simultaneously.

Second, research must translate life-course data into practical tools that support early intervention and prevention.

Third, policymakers should create enabling environments that support cross-sector coordination, including health, social care, and community services.
For public health researchers and policymakers, the implications are clear. We must design systems that reflect the complexity of real lives, not simplified models of disease. We need to prioritise coordination across sectors and across the life course. And we need to ensure that lived experience informs every stage of decision-making.

This webinar demonstrated that systems thinking and joined-up approaches to healthy ageing are feasible. However, success depends on shifting from isolated actions to coordinated systems, and from abstract frameworks to approaches grounded in the realities of people’s lives.
The STAGE project aims to demonstrate the importance and feasibility of a life-course approach to support healthy ageing and to integrate this knowledge into transferable person-centred solutions to add healthier years to people’s lives.
If you missed the webinar, watch the recording below.
Written by Ximena Ramos Salas
